Breast Reconstruction in Huntsville, AL
Mastectomy
Mastectomy is one of the most common treatments for breast cancer and it involves the surgical removal of breast tissue. Patients who are at high risk of developing breast cancer may also undergo this procedure as a preventive measure. Depending on the patient’s individual circumstances, breast reconstruction may be performed at the same time as the mastectomy, or reconstruction may be delayed until after the patient has healed and/or additional cancer treatments have been performed.
Breast Reconstruction
Breast Reconstruction is a process that seeks to restore a woman’s breast (one or both) to a natural shape, size and appearance. Many women desire the results of breast reconstruction to appear similar to their breasts original appearance, but each patient can choose how she would like the results of her reconstruction to look and feel. If only unilateral (single side) mastectomy and reconstruction are planned, a breast lift, breast reduction or breast augmentation can be performed on the opposite breast
to make the breasts appear as symmetrical as possible.
Breast reconstruction can help reduce the physical and emotional effects of having partial or all breast tissue removed by restoring a more feminine shape to the breast and improving the woman’s self-image. Choosing to undergo breast reconstruction is a highly personal decision, and patients should decide based on their own desires rather than outside influences.
The Women’s Health and Cancer Rights Act of 1998 is a federal law requiring insurance plans that provide benefits for mastectomy for cancer to also provide coverage of all stages of reconstruction. This mandate includes surgery of the unaffected breast in order to attain a more symmetrical appearance. This law applies to all types of breast reconstruction after total mastectomy (lumpectomy excluded),regardless of surgical option chosen and whether done in conjunction with a mastectomy or, at a later date (delayed breast reconstruction). Dr. Knowling will work with your surgical oncologist to provide an optimal reconstructive experience.
Breast Cancer support groups can be instrumental in helping the patient with a recent breast cancer diagnosis understand the process of recovery after mastectomy including aspects of breast reconstruction.
Niple Reconstruction
Various techniques are available to preserve or reconstruct the nipple and areola. During your consultation, Dr. Knowling will explain all of the options available to you. Recent developments in reconstruction seek to preserve the breast skin and nipple-areolar complex. Whether a patient is a candidate for breast conservation within the context of reconstruction after mastectomy will be determined by Dr. Knowling and their oncologic surgeon.
Implant vs. Tissue Flap
Expander and Implant Reconstruction
Most breast reconstruction procedures currently performed involve the placement of an implant. A tissue expander is temporarily inserted into the breast pocket after mastectomy to stretch the remaining breast skin and usually also the underlying muscle so that it can adequately cover an implant. Additional tissue may be added. Over the course of several weeks, the expander is progressively filled with a saline solution or air through an internal valve as an in-office procedure, performed usually every
two weeks. Once the tissue is stretched enough, the expander is removed during a second procedure (hospital/out-patient) and replaced by a breast implant. This technique takes longer to achieve the final breast reconstruction than the tissue flap method, but it allows for an easier recovery.
Tissue Flap Reconstruction
This method of reconstruction uses tissue from another area of the patient’s body, such as the back, thigh or abdomen, to reconstruct the breast mound or to provide enough tissue to cover an implant. The new breast tissue may remain connected to the original blood supply through blood vessels tunneled beneath the skin to the donor site, or it may be detached and rely on the growth of new blood vessels (tissue graft). If the flap is being used to provide tissue coverage, an implant or tissue expander
may be inserted beneath.
Immediate or Delayed Breast Reconstruction
Dr. Knowling in conjunction with your breast cancer team of physicians will determine the most appropriate timing of your reconstructive surgery. Immediate breast reconstruction involves working with your breast surgeon at the time of mastectomy. Suitability for this procedure will depend on the nature of the breast cancer and the likely need for subsequent cancer treatment. Delayed breast reconstruction is performed after all other cancer treatments have concluded and the patient has
recovered. The decision for the timing of this procedure is made by Dr. Knowling in conjunction with your oncologic surgeon and your cancer therapy teams.
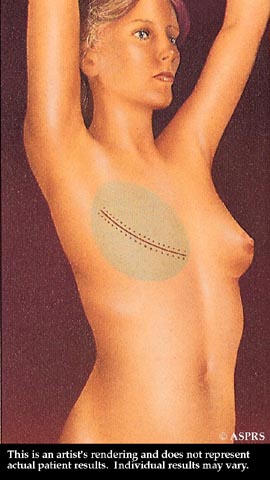 A tissue expander is inserted following the mastectomy to prepare for reconstruction.
A tissue expander is inserted following the mastectomy to prepare for reconstruction.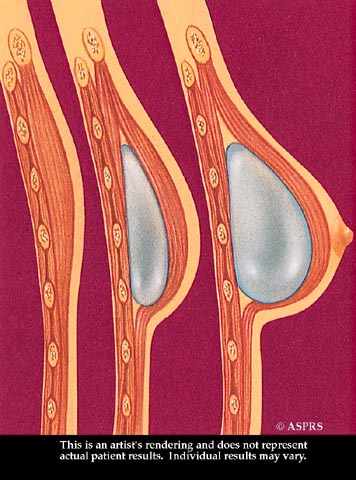 The expander is gradually filled with saline through an integrated or separate tube to stretch the skin enough to accept an implant beneath the chest muscle.
The expander is gradually filled with saline through an integrated or separate tube to stretch the skin enough to accept an implant beneath the chest muscle.
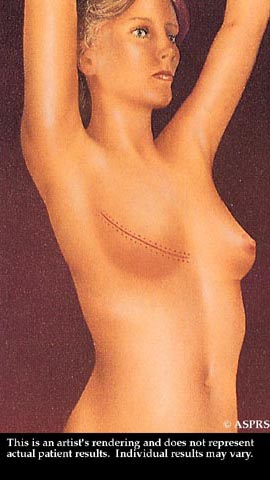 After surgery, the breast mound is restored. Scars are permanent, but will fade with time. The nipple and areola are reconstructed at a later date.
After surgery, the breast mound is restored. Scars are permanent, but will fade with time. The nipple and areola are reconstructed at a later date.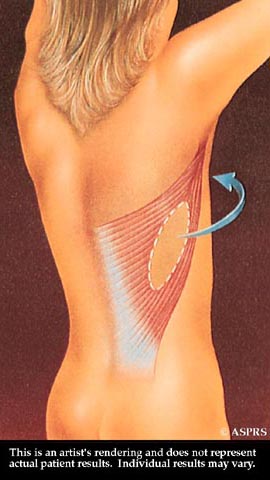 With flap surgery, tissue is taken from the back and tunneled to the front of the chest wall to support the reconstructed breast.
With flap surgery, tissue is taken from the back and tunneled to the front of the chest wall to support the reconstructed breast.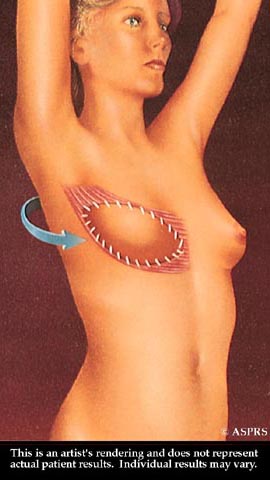 The transported tissue forms a flap for a breast implant, or it may provide enough bulk to form the breast mound without an implant.
The transported tissue forms a flap for a breast implant, or it may provide enough bulk to form the breast mound without an implant.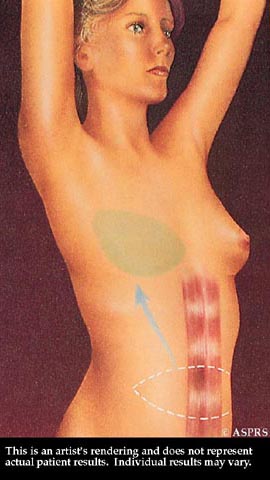 Tissue may be taken from the abdomen and tunneled to the breast or surgically transplanted to a new breast mound.
Tissue may be taken from the abdomen and tunneled to the breast or surgically transplanted to a new breast mound.
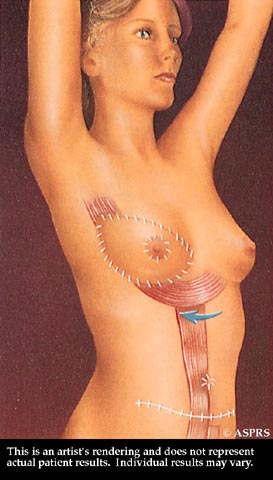 After surgery, the breast mound, nipple, and areola are restored.
After surgery, the breast mound, nipple, and areola are restored.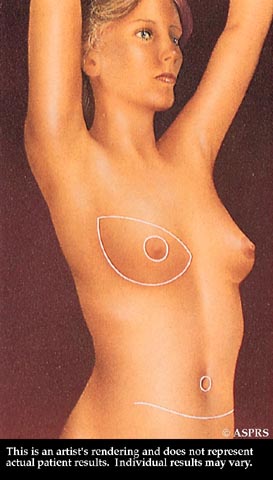 Scars at the breast, nipple, and abdomen will fade substantially with time, but may never disappear entirely.
Scars at the breast, nipple, and abdomen will fade substantially with time, but may never disappear entirely.Have additional questions about the Breast Reconstruction in Huntsville, AL procedure? Schedule a Consultation with Dr. Knowling for further information.